Health Insurance Verification Built to Boost Your Wallet
Faster Payment Determination, Collections and Reimbursement
Clearwave's Multi-Factor Eligibility™ drives cleaner data, reduced claim rejections and instant co-pay determination — meaning more money in your pocket. Don't just keep up, accelerate your cash flow while reducing the hours it takes for staff to verify insurance — you can even reallocate those FTE resources to other areas of the practice. Present the most accurate co-pay at every patient check-in, increasing collections by 112%, while reducing claim rejections by 94% and workloads by 2x.
Fast, Accurate Health Insurance Verification Software
Switching to Clearwave Eligibility Saves Time & Money
When practices implement Clearwave Eligibility they see immediate and long-term results.
From staff cost and time savings to dropping claim rejections, see what your practice could be missing out on!
Additional Revenue Per Provider
By reducing no-shows, dropping claim rejections and increasing collections at the point-of-service.
Drop in Claim Rejections
With faster eligibility verification and improved patient data capture, solving issues before they halt revenue.
Staff Hours Saved
By reducing workloads and reallocating eligibility and benefits employees to other areas, while reducing backfill needs.
Clearwave's Health Insurance Verification Benefits
Get Paid More & Drop Costs
Stop chasing down co-pays after patients come in for their appointments and reduce refunds, resubmissions and other overhead costs. Help your practice do more, with less staff involvement and billing setbacks — see what your practice is missing without Clearwave Multi-Factor Eligibility.
Increase Payments, Reduce Refunds and Rejections
Clearwave's Health Insurance Verification Benefits
Stop chasing down co-pays after patients come in for their appointments and reduce refunds, resubmissions and other overhead costs. Help your practice do more, with less staff involvement and billing setbacks — see what your practice is missing without the leading health insurance verification solution on the market.
What is the best way to give staff a real-time view of patient insurance?
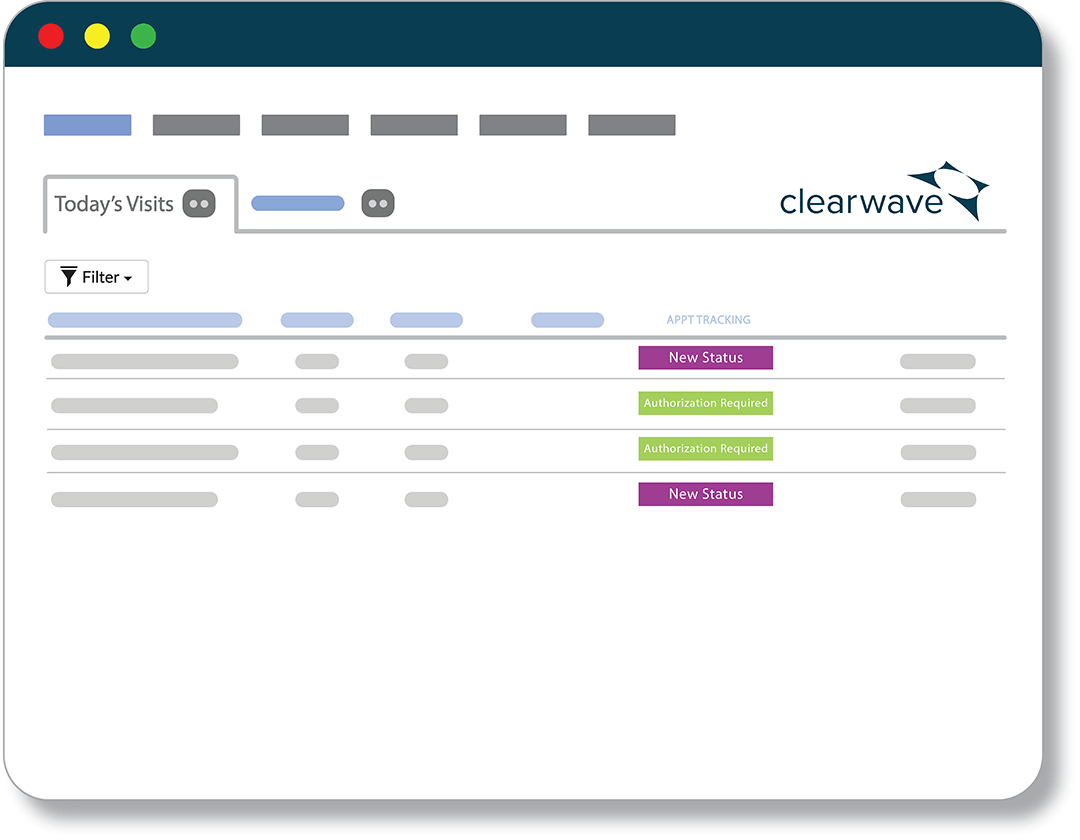
Clearwave's eligibility dashboard provides a real-time, all-patient view of insurance verification statuses in a single click, eliminating the need for staff to check each patient record individually.
How to reduce manual health insurance verification burden?
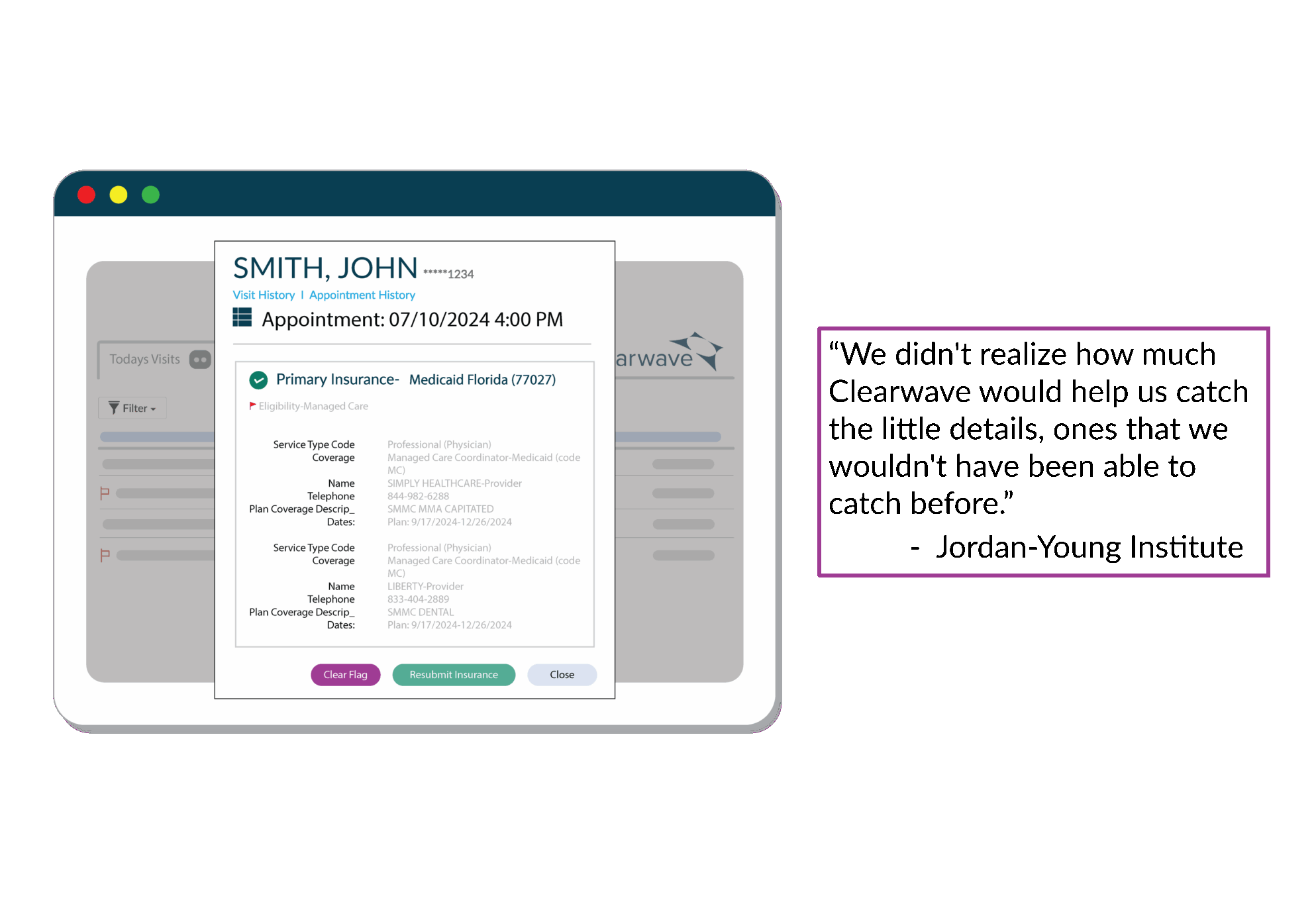
Clearwave's unique flagging system instantly alerts staff to patients with insurance discrepancies that require action — turning hours of manual review into minutes of targeted follow-up.
How to speed up Vision vs Medical authorizations?
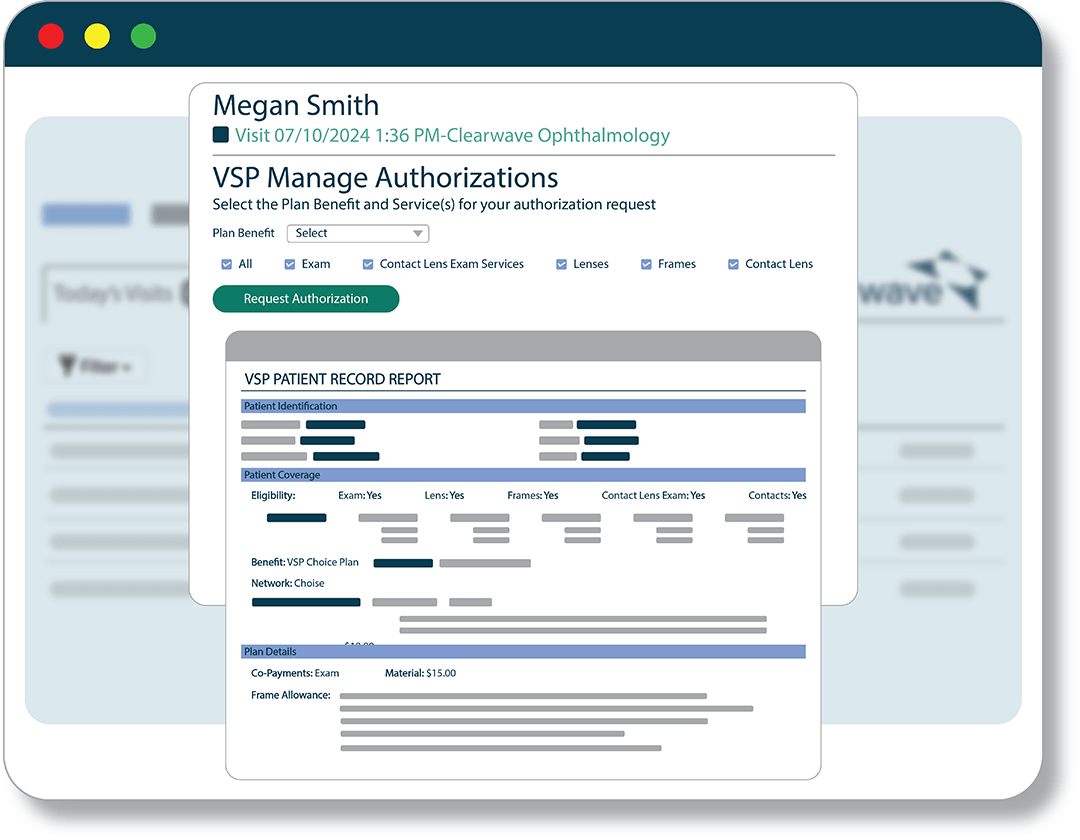
With a direct connection to Eyefinity, Clearwave will determine when to collect from the Vision co-pay vs. Medical, in real-time, streamlining collections and reimbursement for ophthalmology practices.
How to increase patient self-pay collections?
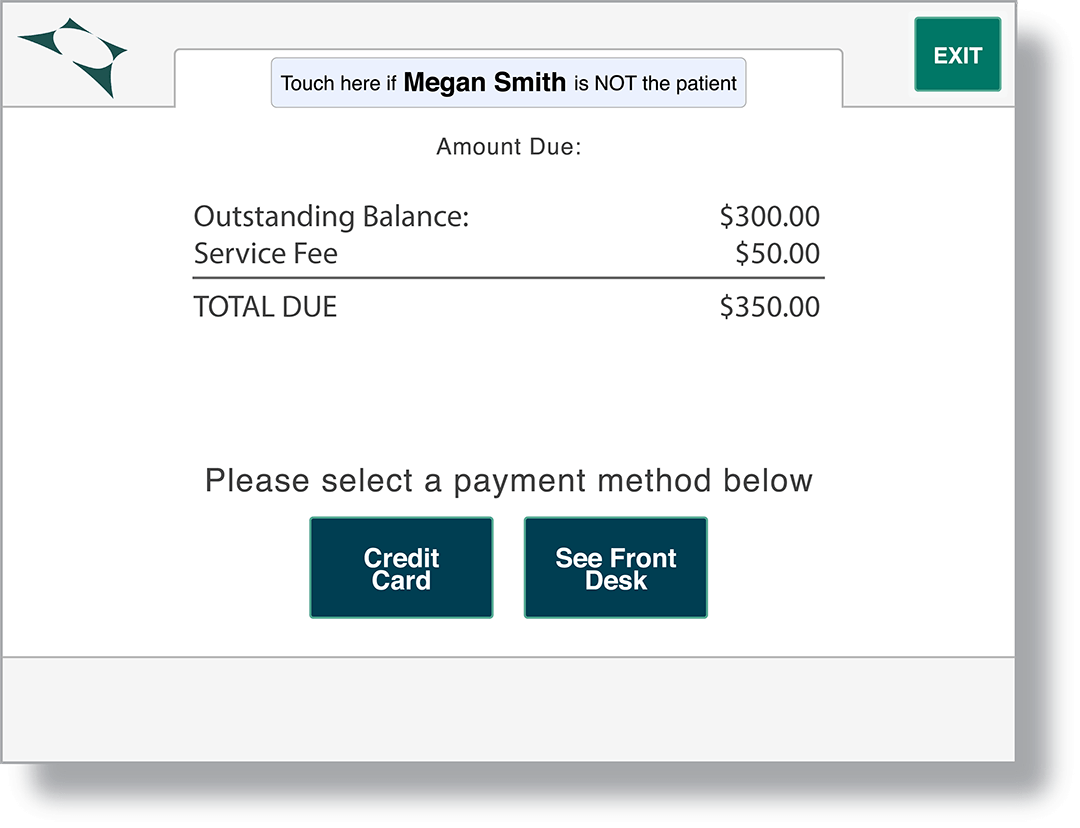
Clearwave can digitally collect self-pay amounts—per the scheduled appointment service—during patient check-in, boosting payments and reducing billing stalls.
How to simplify Medicaid verification for staff?
Clearwave's eligibility engine checks self-pay patients against Medicaid coverage in real-time and flags discrepancies instantly, helping billing teams catch errors before they become claim rejections.
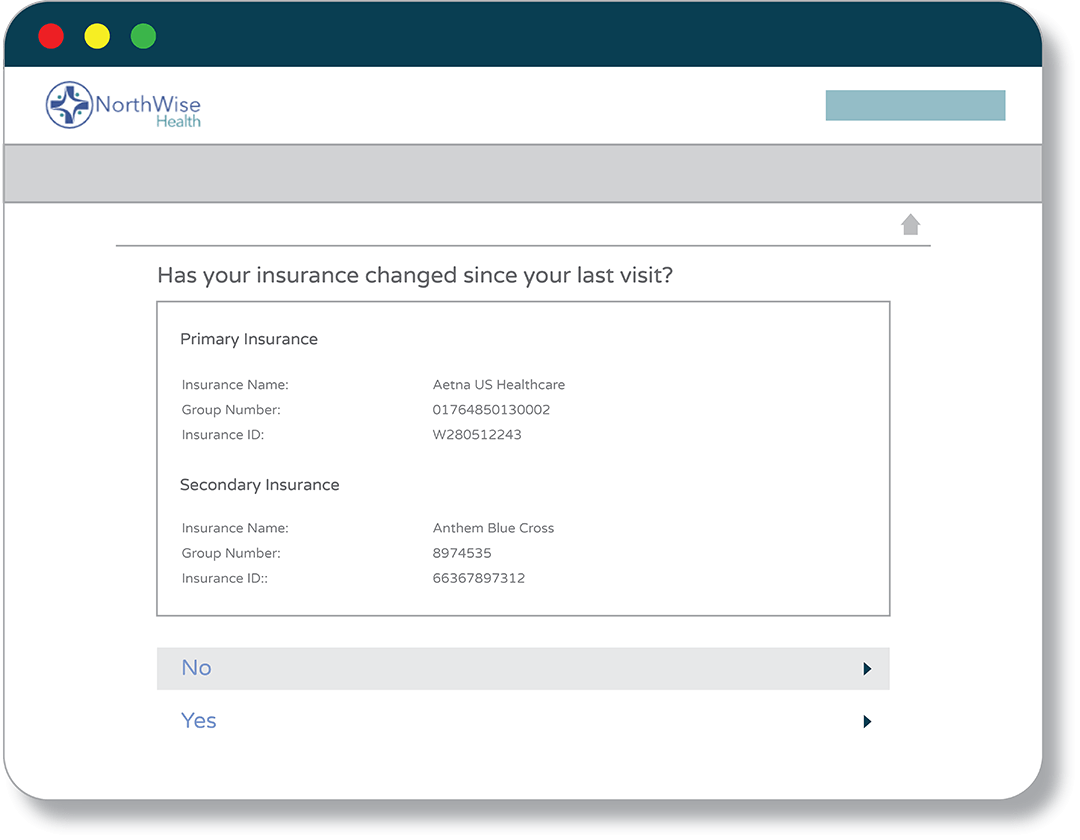
Should patient eligibility be verified during booking?
Yes, Clearwave Scheduling automatically runs eligibility checks during appointment booking and alerts patients to insurance errors on the spot, catching billing issues long before they reach your back-end team.
See the Power of the Clearwave Dashboard
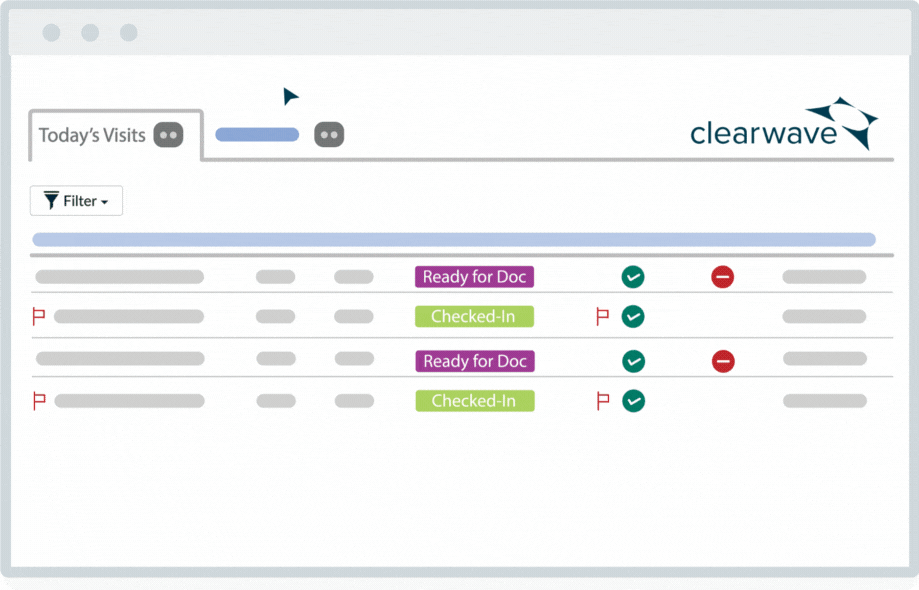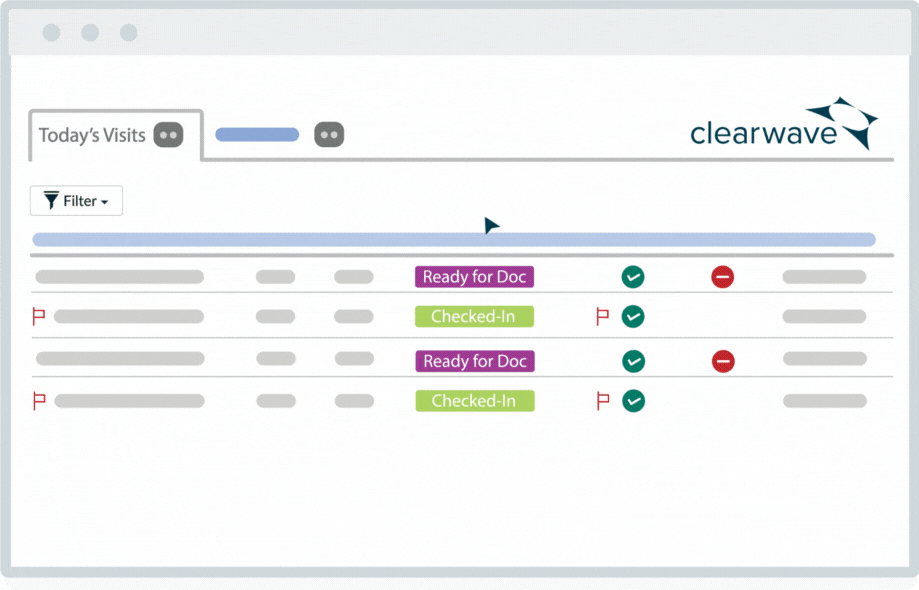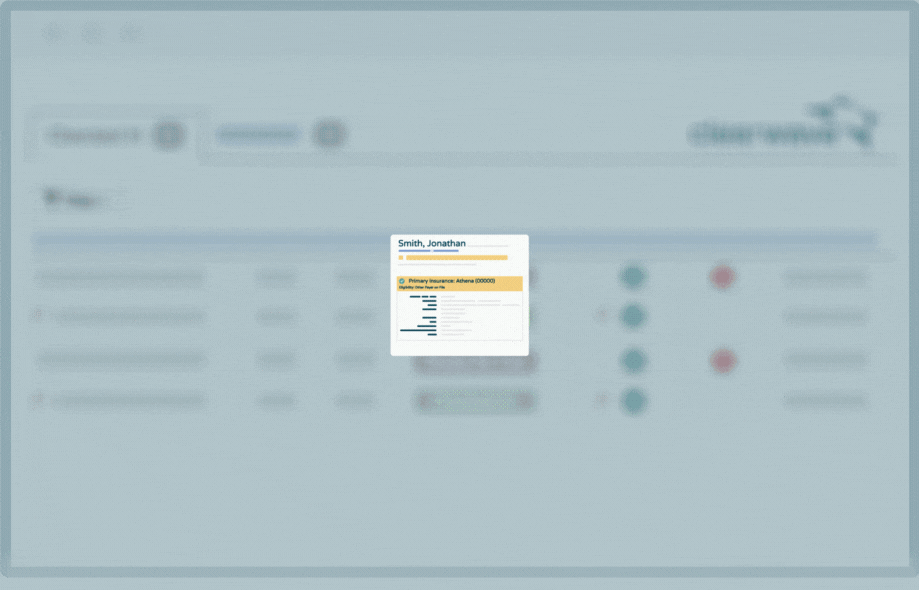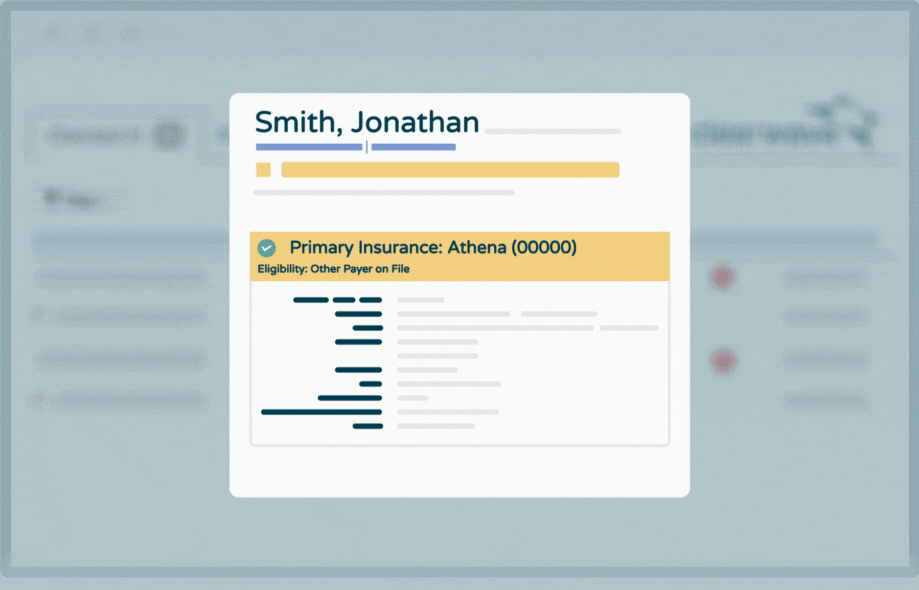
![]() Reconciles today's patients in one single view.
Reconciles today's patients in one single view.
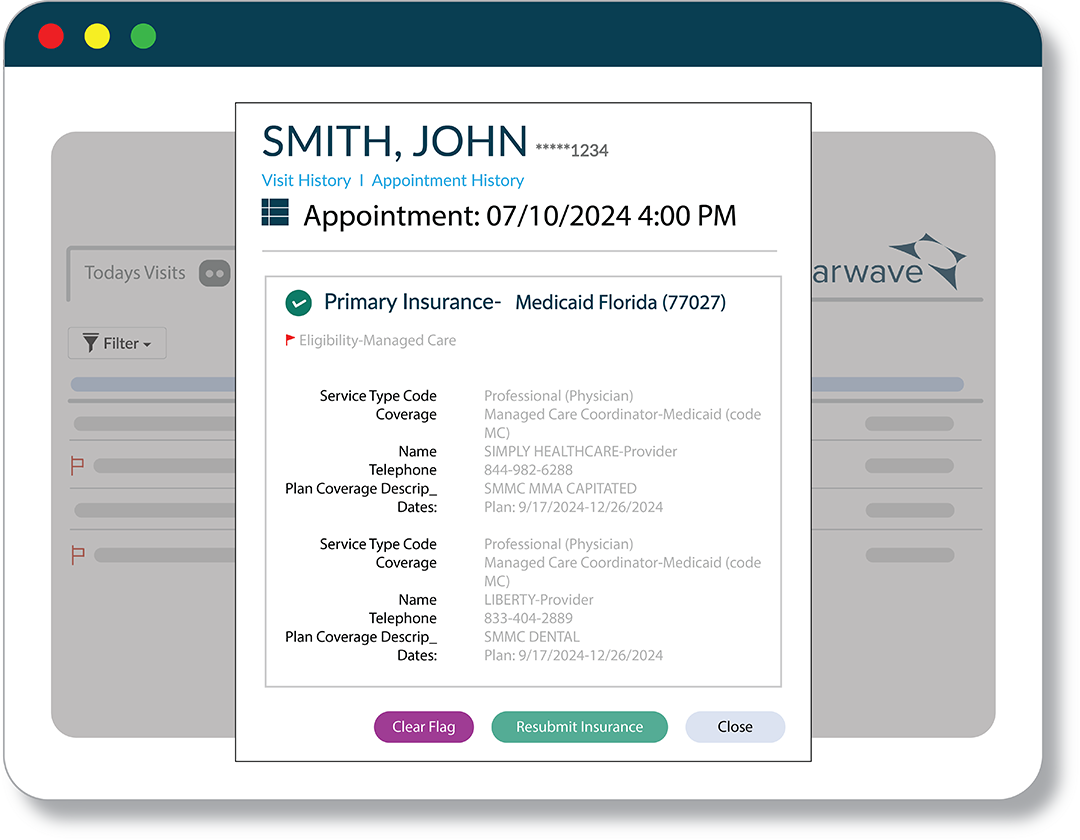
![]() See E&B Report, Co-pay, Data Conflicts and HMO Payers.
See E&B Report, Co-pay, Data Conflicts and HMO Payers.
![]() E&B data displays based on the service being performed.
E&B data displays based on the service being performed.
![]() Includes eligibility status and flags insurance errors.
Includes eligibility status and flags insurance errors.
![]() Filters to show only the patients with eligibility exceptions.
Filters to show only the patients with eligibility exceptions.
![]() Displays vision insurance and associated co-pay.
Displays vision insurance and associated co-pay.
Frequently Asked Questions
About Health Insurance Eligibility Verification Software
Get answers to common questions about verifying patient insurance benefits.
Smart & Seamless
Clearwave Patient Engagement Platform Integrations
Clearwave extends PMS/EMR capabilities to reduce staffing strains while helping you put patients first and reduce profit leaks. With a commitment to innovation and superior client success, you can trust Clearwave to help you navigate the evolving healthcare landscape.
Proven Medical Insurance Verification Software
How Clearwave's Multi-Factor Eligibility Benefits Practices
See the real-world impacts of Clearwave's health insurance eligibility verification software.
Utah Cancer Specialists Put a Stop to Patient Insurance Setbacks
As the largest oncology and hematology treatment practice in their area, Utah Cancer Specialists implemented Clearwave Registration and Eligibility to…
CVG Reduces Claim Rejections & Improves Patient Experience
The CardioVascular Group (CVG) provides cardiology care across 9 locations with 19 physicians who see roughly 500 patients per day….
Thomas Eye Group Case Study
Thomas Eye Group needed a solution to solve long waiting room lines, past due payments and errors in patient data…
Let's Get You Paid - Literally
Connect with our team for a brief solution overview and get $50 - no strings attached.