Your Solution to Increasing Patient Collections
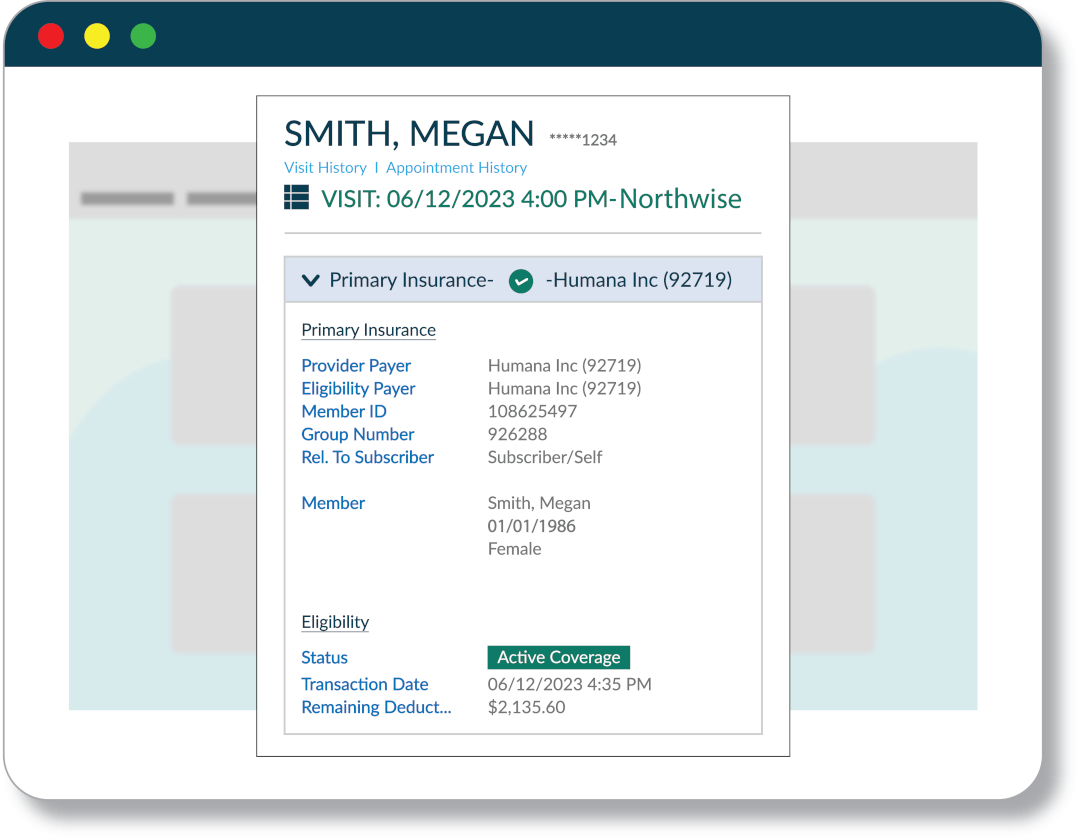
Multi-Factor Eligibility™
Our unique, Multi-Factor Eligibility™ solution is proven to drop staff workloads by increasing efficiency in a way that outperforms other automated verification solutions, by reducing claim rejections by 94% or more!
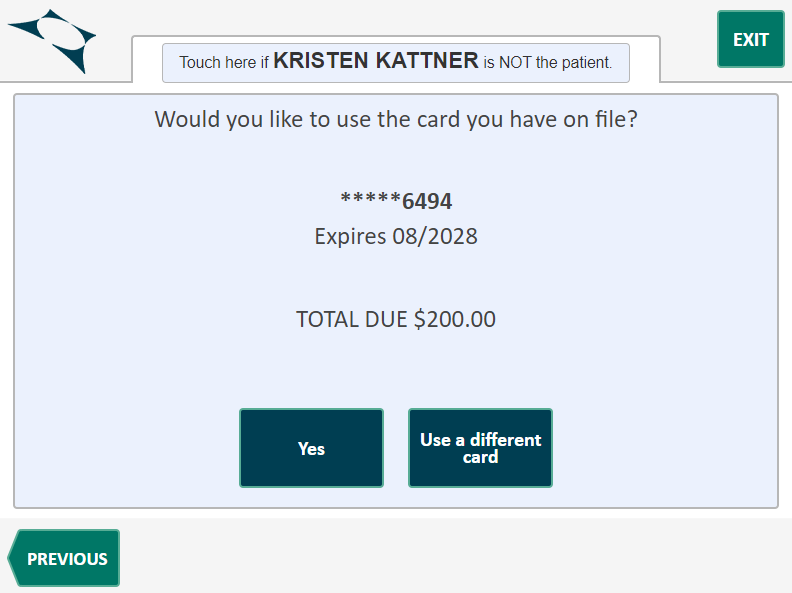
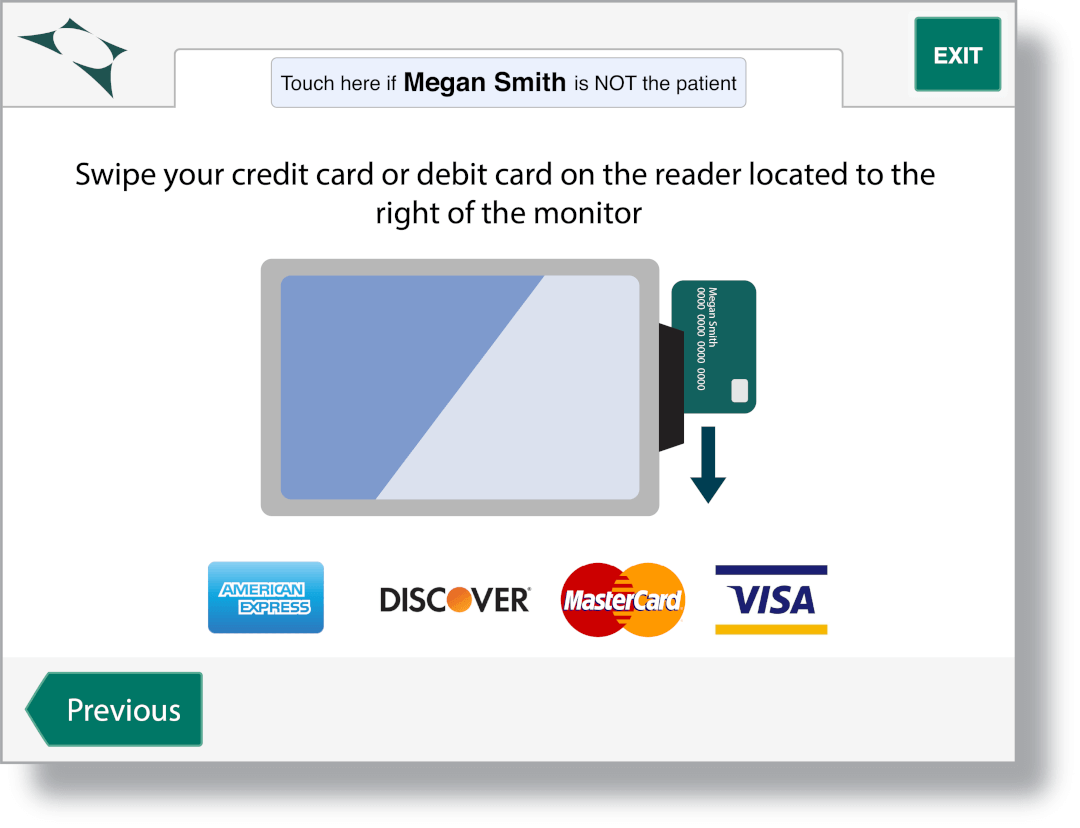
Card-On-File Payments
Collect patient card-on-file information in Clearwave and use that same card to collect payment!
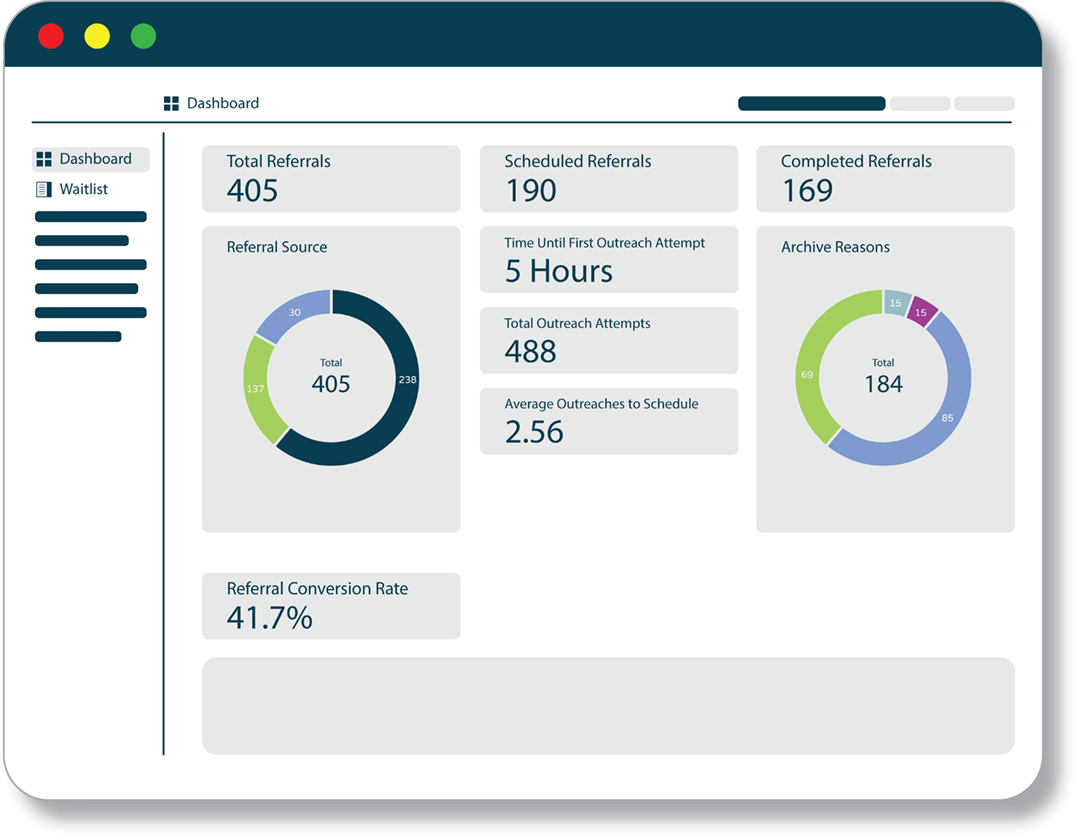
Referral Tracking/Management
Never lose a referral again and ensure patients are booked immediately with automated referral management and tracking that ties directly into Clearwave Scheduling.
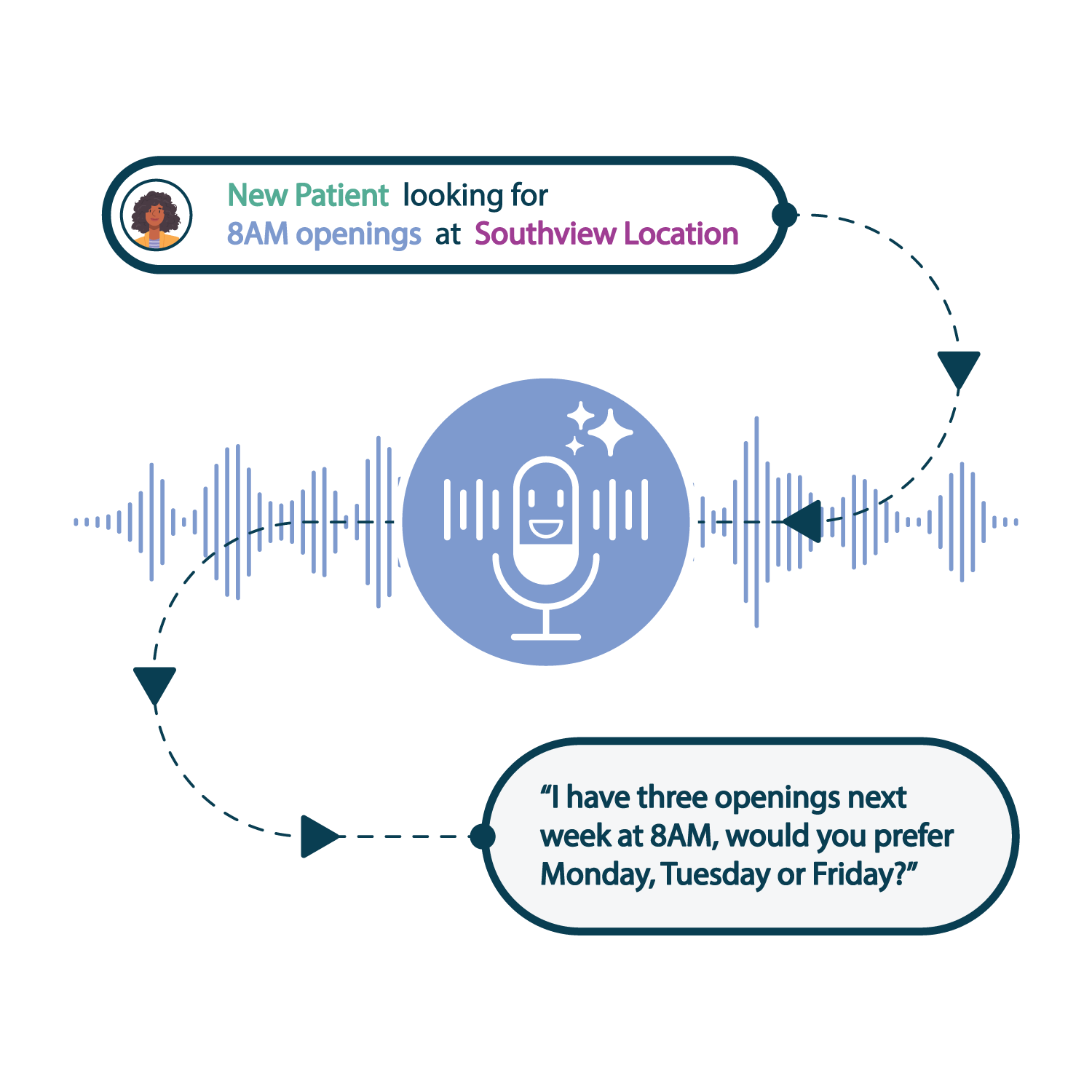
Voice AI
Capture demand for every patient calling in and drop abandoned bookings with Clearwave Voice AI. Drop no-show and appointment gaps with a 24/7 booking AI engine.
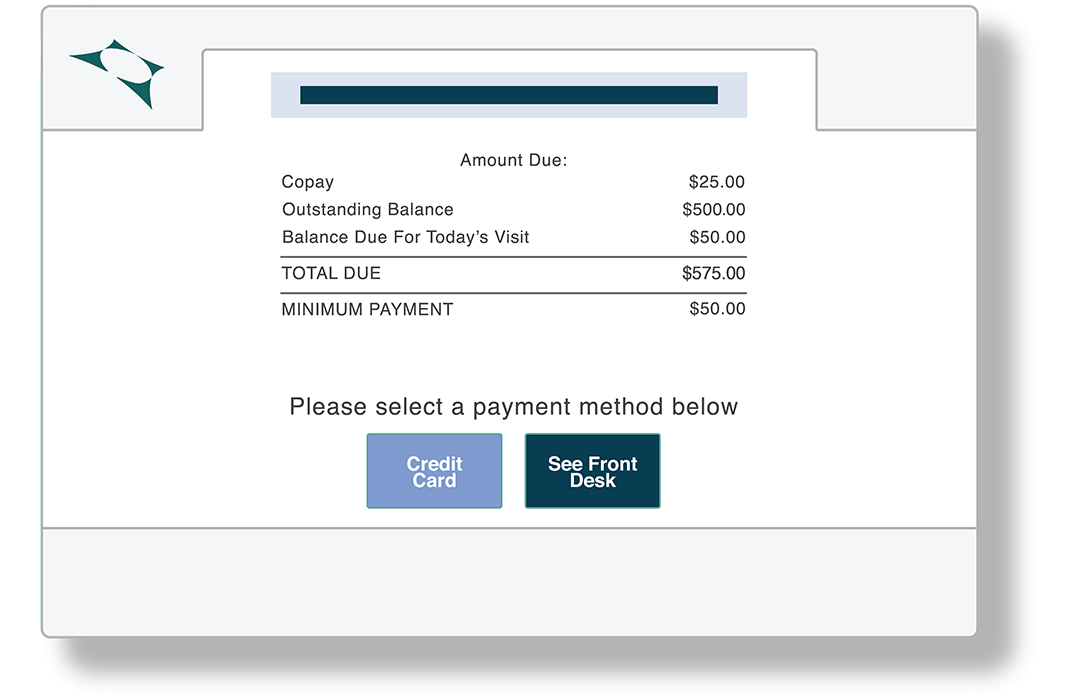
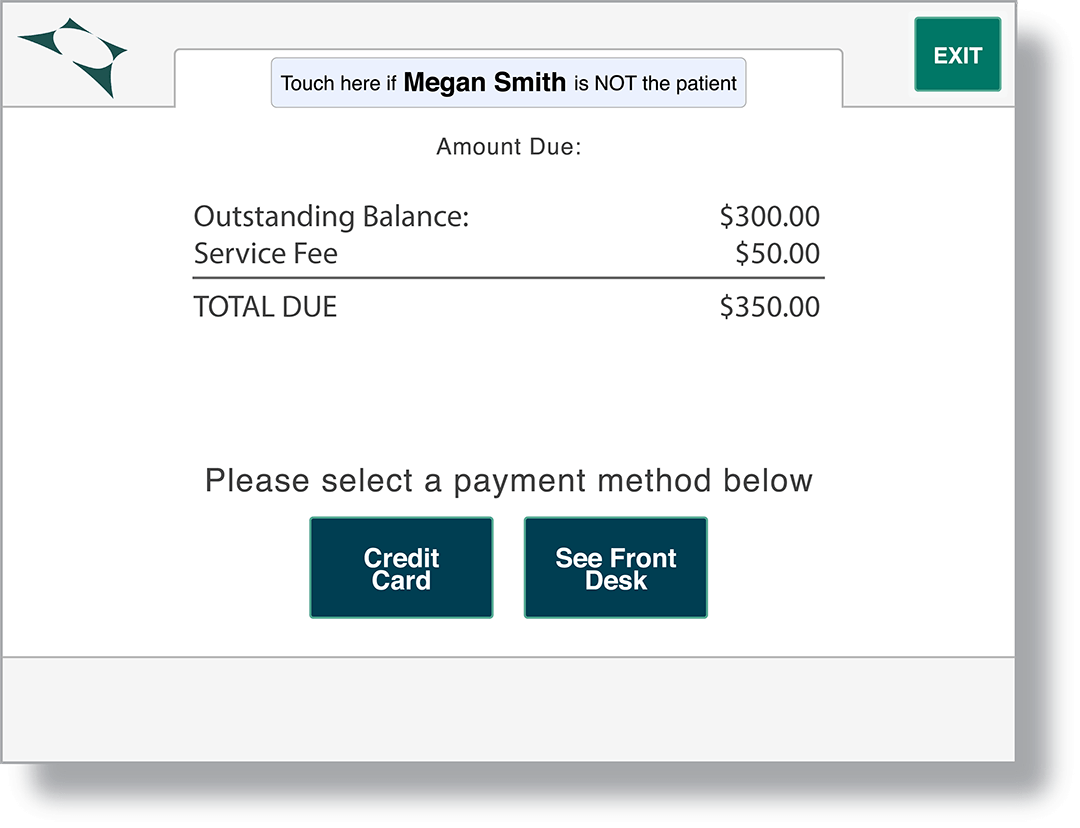
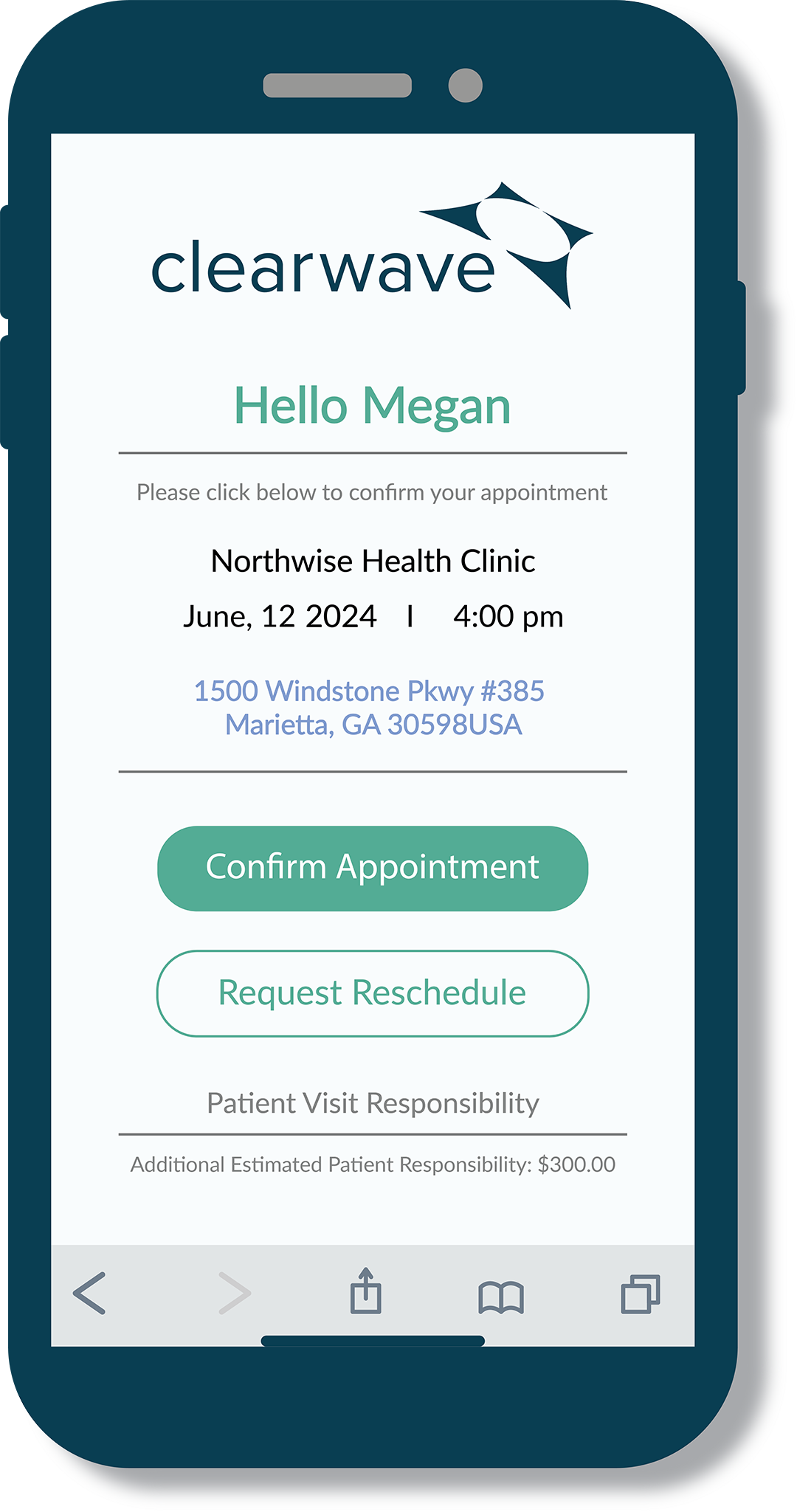
Point-Of-Service Collections
Drop post-service billing costs and effort by increasing your point-of-service collection rate. Digitally collect patient co-pays, past-due and estimated balances instantly during check-in.
Self-Pay Collections
Digitally collect desired self-pay amounts—per the scheduled appointment service—during patient check-in, automatically.
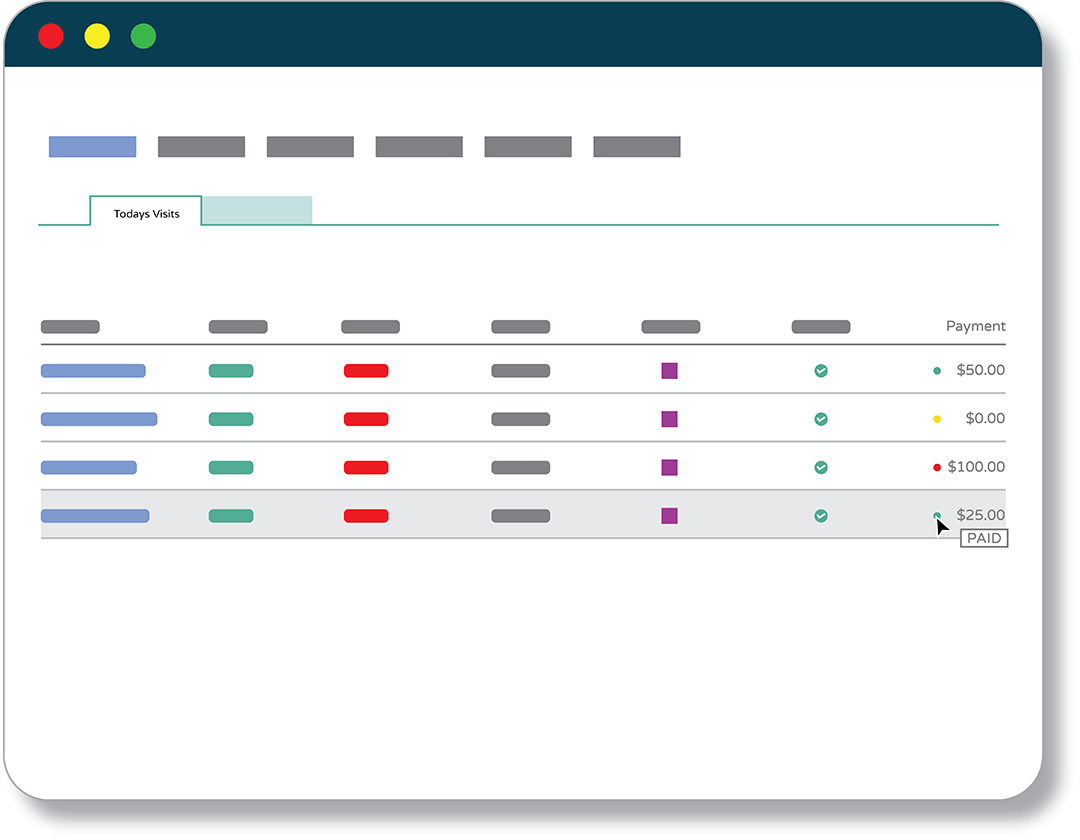
Patient Payment Insights & Trends
Staff can quickly see which patients have/haven’t made payments, what’s owed at check-in and much more. Choose all-patient or individual views and take action to increase collections during check-in.
Estimations Generator
Collect more, faster. Make providing and collecting patient cost estimates a breeze. Powered by Rivet Health.
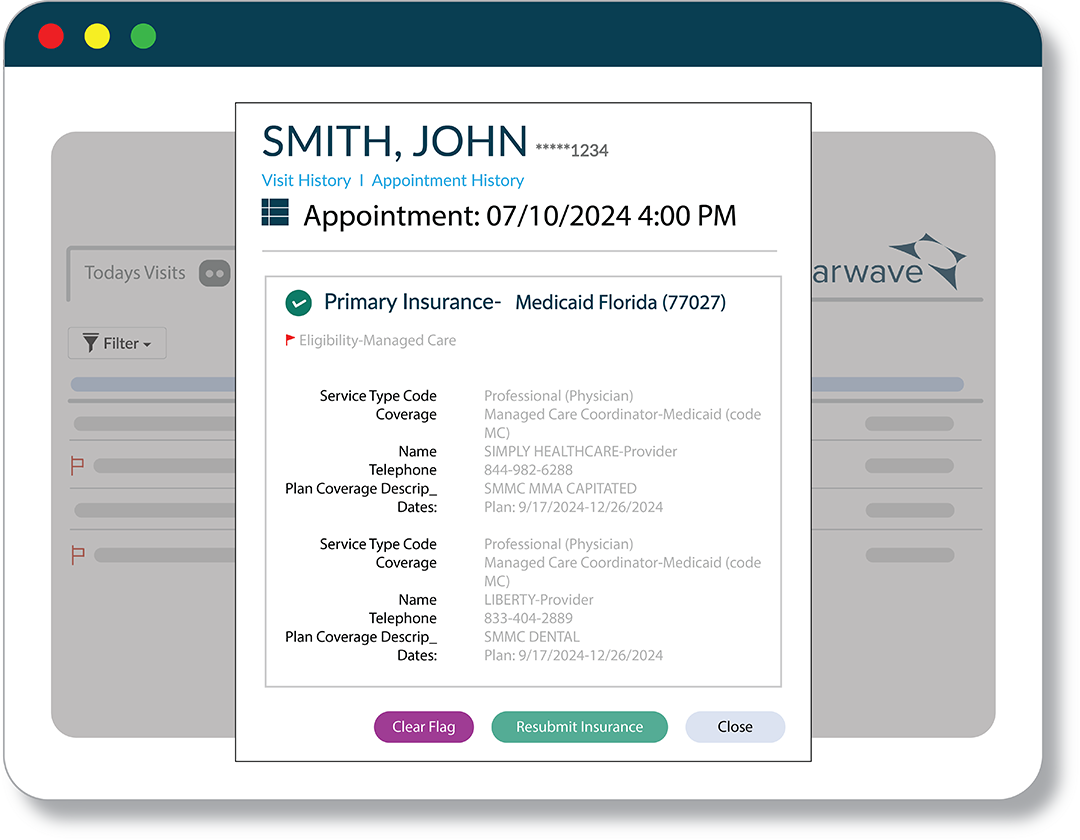
Medicaid Patient Identification
Quickly verify if patients have Medicaid coverage, a managed care plan or a replacement plan.
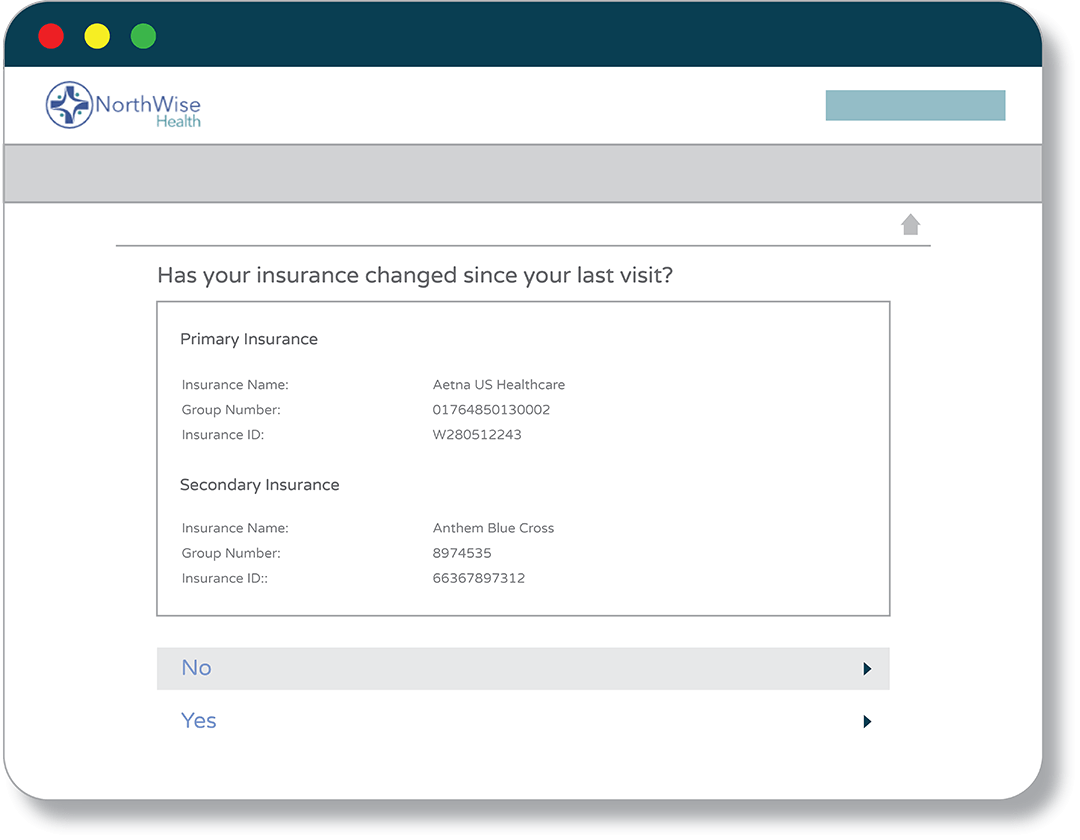
Eligibility at Scheduling
Automatically collect and verify eligibility benefits during appointment scheduling and prompt patients to solve errors ahead of time.
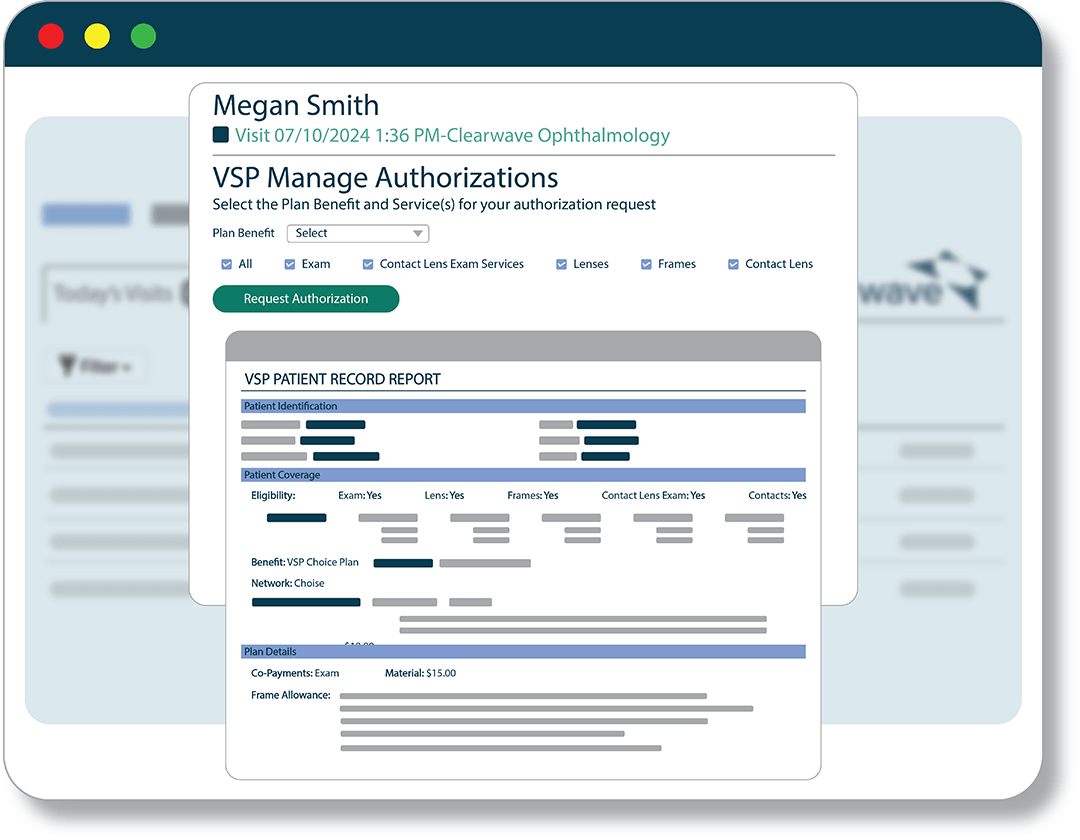
VSP Authorizations
Verify VSP eligibility and manage VSP authorizations through our direct connection to Eyefinity.
Robust Payer Network Ecosystem
Clearwave will automatically resubmit errored eligibility transactions, increasing the number of active insurances returned and reducing claim rejections and staff workloads in one fell swoop.
Real Clients, Real Results, Real Measurable Impact
Frequently Asked Questions About Amplifying Revenue
See How Clearwave Increases Collections at Practices Like Yours
How OSMS Eliminated Check-in Bottlenecks & Grew Collections Along the Way
The Orthopedic & Sports Medicine Specialists of Green Bay (OSMS) matched increasing provider and patient numbers with one solution that…
Metrolina Eye Associates Sees Higher Collections & Happier Patients
After implementing self-registration kiosks, Metrolina Eye Associates saw a 50% drop in check-in times and a nearly 40% increase in…
Utah Cancer Specialists Put a Stop to Patient Insurance Setbacks
As the largest oncology and hematology treatment practice in their area, Utah Cancer Specialists implemented Clearwave Registration and Eligibility to…
Increased Profits at Your Specialty Healthcare Practice!
Enter description text here. Lorem ipsum dolor sit amet, consectetur adipiscing. Quo incidunt ullamco.